
Coming to the end of the active treatment process can often feel like the final chapter in the book for those affected by breast cancer. Whilst for some this may come as a great relief, for many others the question of what life will be like now can become a growing issue. New concerns can begin to crop up as hospital-based care draws to a close such as worries over physical appearance, anxiety about cancer returning and experiencing loneliness.
In this blog we take a closer look at a number of these key concerns and discuss some of the best ways of managing these during this challenging transitional period.
Accepting the Impact of Cancer
Initially, there may be a temptation to strive towards living life as it was before the diagnosis as if nothing has really changed. However, according to oncologist Lidia Schapira, recognising how cancer has impacted your life is a vital stage in the process after treatment:
“The important message is that life may be forever changed by the experience of having cancer, and those changes deserve careful attention and respect”.
– Lidia Schapira, Oncologist1
Here she urges patients to really take into account all of the changes that have occurred since the diagnosis, both major and minor, before attempting to move on. So, what does this mean in practice? Here are a few key areas to focus on:
- Discussing with your doctor the potential physical limitations that you may now have since your treatment.
- Recognising some of the strengths you have gained since your diagnosis; are you more resilient? Are you more connected with loved ones?
- Talking openly with friends and family about how things have changed since your diagnosis and how you see yourself now.
Being open and honest about the ways in which cancer has affected you is key to starting the next step in the process and provides the basis for looking forward to the future.
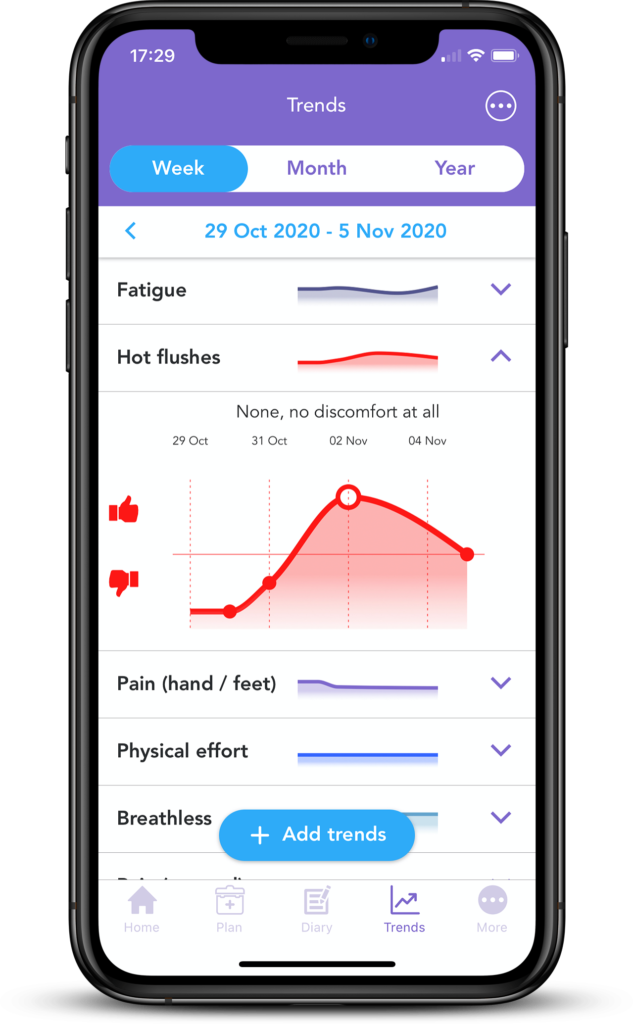
As you approach the end of your breast cancer treatment, it can be difficult to remember and visualise how your symptoms have changed since the very start. With the OWise Breast Cancer App, you can keep a record of how your wellbeing has changed over time, and then review it all at a later date.
Fear of Cancer Recurrence
The fear of cancer recurrence, or cancer coming back, is very common among those who are reaching the end of their active treatment period. The American writer Susan Sontag in her book published in 1978 ‘Illness as Metaphor’ describes the experience of having a cancer diagnosis as having two sides, both the physical and psychological2. This means that while cancer and its treatments have a physical effect on your body, the stigma and fear that is associated with cancer also contributes to the struggle. That may explain why even when cancer is physically gone, the fear associated with it can linger for much longer. To learn more about the fear of cancer recurrence, please check out our previous blog.
In practical terms, you’ll most likely find that you’re spending less and less time in hospitals speaking to doctors. Clearly, different patients respond differently to this reduced medical attention, with some wanting to get their questions answered as soon as possible, and others dreading the thought of going back for a meeting with the doctor. Regardless of how you respond to this, there are a number of ways to work against the fear of cancer recurrence that can make the end of cancer treatment that much easier to manage.
One way is to keep on top of any changes to your body. Having just finished a very stressful period of cancer diagnosis and treatment, it can be a difficult step to start thinking about the signs of recurrence. However, detecting these changes early can improve the treatment options and outlook.
Be aware of these common signs for both cancer recurrence and for secondary breast cancer, but try not to overthink it. Instead, choose a memorable time in your routine when you have some peace, quiet and privacy, and have a check. If you notice anything out of the ordinary, make sure to let your care team know as soon as possible.
Once you’ve had a think about these suggestions and even made a plan about how you’re going to approach appointments and checking symptoms, this doesn’t always mean your fear will automatically disappear. Gabriela Gutierrez, an Oncology Therapist, encourages patients who are in complete remission to try and separate the physical and mental effects of cancer:
“Cancer was able to guide so much of your life during treatment; now that it is out of your body, we don’t want to continue to give it the power to guide you even though it’s gone. That’s not the life you fought for”.
– Gabriela Gutierrez, Oncology Therapist3
Dr. Gutierrez asks patients to look at their lives from a wider perspective whereby cancer only plays a limited part. Therefore, while it’s currently not physically a part of you, by all means make plans for the future with your follow ups and self-checking, but also endeavour to continue living in the cancer-free present.
Changes to the Body and Body Image
“For many women, negative changes in body image become part of the long-term side effects of treatment. This is especially true in women whose body image centres around their femininity”
– Gloria Martinez Ramos, Professor in Sociology4
This kind of self-perception is usually referred to as body image and can certainly impact how we see and express our gender and our sexuality. If you want to explore further the topic of sexuality and breast cancer, please check out our previous blog on sex and intimacy.
Here we will look at some ways to help resolve this internal conflict and alleviate some of these issues surrounding body image, both through conversations with others and with yourself.
Speaking about your thoughts and feelings
Whether it’s with your doctor, or with friends and family, speaking about how the physical changes to your body are affecting your body image can lead to a lot of benefits both for you and for them. It can help lighten the load and make it easier for those on the outside to understand your position. You can also reach out to others with similar experiences, though we will discuss this further in the next section.
When it comes to sex and intimacy, speaking with your partner about your body image and how you see yourself can help them understand your position and even help to explain any hesitation you have. Once you’re on the same page it can be easier to discuss how you imagine your sex life changing overtime.
“The app gave me a familiar feeling in a difficult time of continuously changing faces and feelings, and registering my emotions in the app helped me to express feelings that I would have otherwise kept to myself” – Young-Afat et al., 20167
Practising self-compassion and patience
Self-compassion is an attitude to oneself that is non-judgemental and accepting of one’s imperfections. One study conducted with over 250 women who had completed their breast cancer surgery, showed that those who showed more self-compassion were less likely to experience anxiety or depression concerning their bodies one year on5. One way of practising this is by writing down how you would talk to someone else if they were in your position. You may find that you do not often treat yourself with the same patience and kindness as you do others.
When it comes to intimacy, during your private moments you can also spend some time discovering which areas and positions are the most comfortable for you. This can help when you choose to become intimate with a partner at a later stage.
Reaching out to the Community

Seeing as this new leg of the journey is such a big change of pace from the regular treatment process, it can initially feel very overwhelming. There are a lot of new things to consider and the people around you, even if they were there to support you through the experience, may not themselves totally understand what you’re feeling now.
This can be a lonely experience so establishing a network of people with similar experiences with whom to discuss, support and compare notes, can make all the difference. One clear way of achieving this is by having a search for a local breast cancer support group or an online community. These are great spaces for sharing your feelings with people who are bound to understand, and who might be able to offer some strategies for coping with your new concerns.
Keep in mind that if you are already part of a breast cancer community or group, you are usually allowed to remain a member even if you have completed your active treatment, so you can still attend the same meetings with the same people. As well as this, it can be a good idea to organise with your peers to meet outside of the group. This way you can speak about different topics and further develop your personal relationships.
Finally, you could also consider the prospect of supporting others who have recently received their diagnosis or started their treatment, either through volunteering or by some other means. Using your own knowledge of your treatment to support someone else can be incredibly beneficial to them. Whilst doctors can outline the various treatment pathways, they usually can’t provide advice based on their own experience.
A review of 13 separate studies on peer support among cancer patients has shown that:
“[Cancer survivors] have an authentic knowledge of what it is like to live with cancer, and as such, they are able to bring a unique perspective to the support process”
– Meyer et al., 20146
Beyond the benefits to the newly diagnosed individual, there can also be a positive outcome for you. Helping out a new patient, either in a voluntary capacity, or using your own professional skills to help out, can be very rewarding and give you a strong sense of purpose. Here are some options you might like to consider:
Read More
Life After Breast Cancer Treatment
Cancer survivors: Managing your emotions after cancer treatment
References
[1] Cancer.net (2019) What Comes After Finishing Treatment: An Expert Q&A [online]. Available at: https://www.cancer.net/survivorship/life-after-cancer/what-comes-after-finishing-treatment-expert-qa
[2] Sontag, S. (1978) Illness as Metaphor, Farrar, Straus and Giroux.
[3] Healthline.com (2020) 5 Tips for Coping with Fear of Breast Cancer Recurrence [online]. Available at: https://www.healthline.com/health/breast-cancer/5-tips-for-coping-with-fear-of-breast-cancer-recurrence
[4] Medpagetoday.com (2017) Body Image and Self Esteem in Women with Breast Cancer [online]. Available at: https://www.medpagetoday.com/resource-centers/breast-cancer-advances/body-image-and-self-esteem-women-breast-cancer/740
[5] Przezdziecki, A., Sherman, K. A., Baillie, A., Taylor, A., Foley, E., & Stalgis‐Bilinski, K. (2013). My changed body: breast cancer, body image, distress and self‐compassion. Psycho‐oncology, 22(8), 1872-1879.
[6] Meyer, A., Coroiu, A., Korner, A. (2015). One-to-one peer support in cancer care: A review of scholarship published between 2007 and 2014. European Journal of Cancer Care, 24, 299-312.
[7] Young-Afat, D. A., van Gils, C. H., Bruinvels, D. J., van der Pol, C. C., Witkamp, A. J., Sijtsema, S. & van den Bongard, D. H. (2016). Patients’ and health care providers’ opinions on a supportive health app during breast cancer treatment: a qualitative evaluation. JMIR cancer, 2(1), e8.
