
Want to be more breast aware or would you just like to know more about breast cancer signs and diagnosis? You’ve found the right place. Let us take you through how to check your breasts, the key signs to look out for, and the process of breast cancer diagnosis in this first part of this blog series.
Breast cancer is the most commonly diagnosed cancer worldwide and each year more than 2.3 million individuals are diagnosed with the disease1. Research suggests that the occurrence of breast cancer is increasing in many parts of the world1. This can be alarming, but it is important to note that detecting breast cancer early significantly increases the chances of beating a breast cancer diagnosis.
Why is detecting breast cancer early important?
The American Cancer Society suggest that when patients are diagnosed with early localised invasive breast cancer (without signs of spreading outside of the breast), 99% of these patients are expected to be alive five years after their diagnosis2. This is an overwhelmingly positive statistic that highlights how important it is to be aware of the signs and symptoms of breast cancer to ensure its detected early.
What is breast awareness?
Being breast aware is knowing what is normal for your breasts. Being familiar with how they normally feel and look can help you to notice any changes that are unusual for you as early as possible.
“I think this is so important and am a huge advocate of checking your breasts and pecs regularly and knowing your normal. I always say to people that you are checking yourself regularly, not to find cancer, but to know your normal, so if anything changes you can get it checked quickly.” – Carly Moosah, Breast Cancer Survivor
How do I check my breasts?
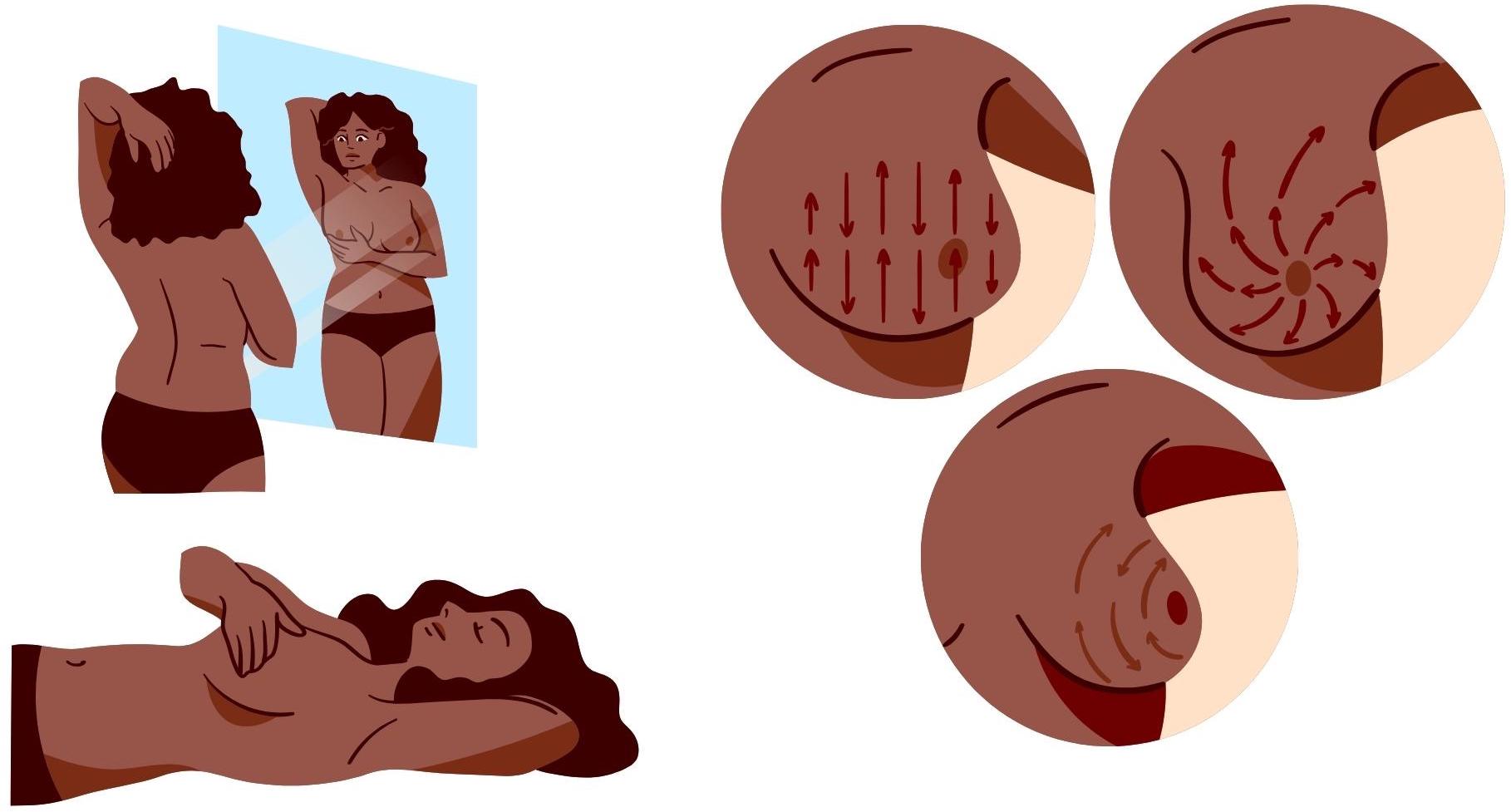
You can check your breasts somewhere that you feel comfortable, such as in the shower or lying down in bed. It can be helpful to do this in front of a mirror. Start by looking and feeling each breast using your fingers to gently press around the tissue3. Make sure that you cover the whole breast and the surrounding area, including up to the collarbone and the armpit. Try to use varying pressure levels and follow some kind of pattern to make sure everywhere gets checked4. Remember to take your time, it is important not to rush so that you examine your breasts properly. It is recommended to check your breasts once a month5.
What are the key signs of breast cancer to look out for?
While you examine your breasts there are many things that can appear unusual, it is important to remember that the majority of lumps found are not cancerous6. Lumps found could be due to a number of reasons including cysts, fibroadenomas and infection7. Additionally, breasts can change depending on the menstrual cycle or with age.
See below the key signs to look out for that could be indicators of breast cancer4,7.
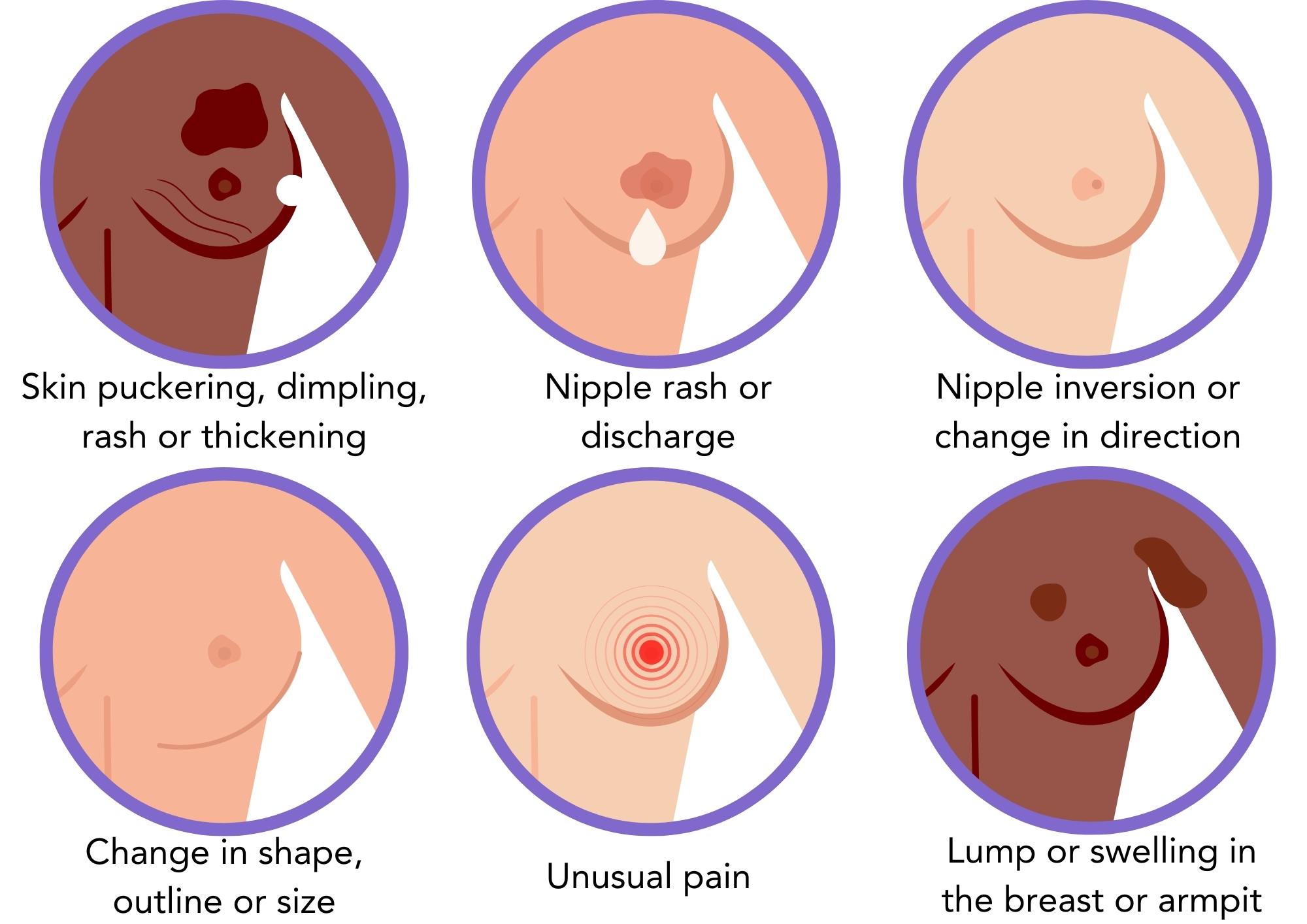
Breast changes you can see:
- Skin puckering, dimpling, rash or thickening
- Nipple discharge, inversion, change in direction, rash or crusting
- Changes in breast shape, outline or size
- Swelling in the armpit or around the collarbone
Breast changes you can feel:
- Lumps, thickening or swelling in the breast or armpit
- Unusual pain in the breast or armpit that does not go away
When should I go to the doctor?
If you find anything out of the ordinary or if you are concerned, you should make an appointment with the doctor. It is important not to panic at this stage. Although being breast aware and self-examinations are key to knowing your normal and detecting any irregularities early, further examinations by a doctor are needed to diagnose breast cancer.
The doctor will perform a physical exam to evaluate whether further testing is needed. This usually consists of checking8:
- The breasts and lymph nodes for lumps or other abnormalities
- The skin on the breasts
- The nipples for inversions, discharge or other abnormalities
You may be asked about your family history to see if there is a history of breast cancer in your family. This could mean that there is a faulty gene in your family that may increase the risk of certain types of cancer, such as the BRCA genes.
If the doctor decides that further testing is needed to investigate changes in the breast, they will refer you to a specialised breast clinic.
What is breast cancer screening?
Breast cancer screening is when women with no symptoms are tested for breast cancer. This aims to detect breast cancer early when it is more treatable. The NHS reported that out of the 2 million women screened each year, around 21,000 cases of breast cancer are detected9. They also stated that the screening programme saves around 1,300 lives per year in the UK10.
Breast screening involves having a mammogram, which takes an image X-ray of the breasts. The breast is flattened between two plastic plates while the X-ray is taken to spread out dense breast tissue and ensure clear images. This process will be repeated to get an X-ray image of the side of the breast.
Having routine mammograms is beneficial to enable the radiologist to compare your most recent mammogram to previous ones to look for changes. Research suggests that those who have regular routine mammograms are up to 25% less likely to die of breast cancer than those who do not have mammograms11. Generally, women receive their invitation to screening around the age of 50, but this can vary from country to country.
If the result is abnormal it does not necessarily mean that you have breast cancer. Further testing is needed to determine whether the abnormality is cause for concern.
How is breast cancer diagnosed?
After your doctor has referred you to a breast specialist clinic or you received abnormal results during breast screening more tests are needed to determine whether you have breast cancer. This is usually done through a triple assessment, consisting of a physical examination of the breast, imaging techniques and testing samples taken from the breast.
Imaging tests
Imaging techniques are used to diagnose breast cancer and to determine the stage and extent of the cancer. A diagnostic mammogram or an ultrasound scan are the most common imagine techniques used. A diagnostic mammogram is similar to a screening mammogram, but the aim is to examine the breast tissue more closely and more images may be taken.
A breast ultrasound uses sound waves to produce an image of the inside of the breast. An ultrasound may be recommended in those with denser breast tissue, such as women under the age of 35 or in men. Denser breast tissue can make it more difficult to detect breast cancer using images from a mammogram12.
In some cases, magnetic resonance imaging (MRI) can be used if the results of the mammogram or ultrasound were not clear. An MRI machine creates detailed images of the breast using magnetic and radio waves. Sometimes a coloured dye is injected into a vein in the arm to enhance tissues or blood vessels on the MRI images.
Imaging scores range from13:
- 0 – Incomplete test
- 1 – Normal
- 2 – Benign, not cancer
- 3 – Probably benign, uncertain
- 4 – Suspicious, might be cancer (2-95% chance)
- 5 – High chance it is cancer (>95% chance)
- 6 – Biopsy proven cancer
Breast Biopsy
A biopsy is a way to determine whether abnormal tissue is cancer and involves a small sample of cells being taken from the abnormal area in the breast. Often, this is done during the same appointment as the imaging tests and then the sample is sent to the laboratory for analysis.
There are multiple biopsy options available14:
- Fine needle aspiration – uses a thin, hollow needle to extract a sample of tissue
- Core needle biopsy – uses a larger needle to extract a cylindrical sample of tissue
- Vacuum-assisted core biopsy – uses a vacuum to collect multiple tissue samples with a single needle insertion
- Stereotactic biopsy – uses mammograms to guide the placement of the needle to take a sample
- Ultrasound-guided core needle biopsy – uses ultrasound to guide the placement of the needle to take a sample
- MRI-guided core needle biopsy – uses MRI to guide the placement of the needle to take a sample
- Surgical biopsy – surgery to remove a larger tissue sample
A particular type of biopsy may be recommended depending on the size, location or other characteristics of the abnormal area in the breast.
Getting your results
Once the biopsy sample has been analysed the pathologist produces a pathology report that details about their findings. The report is sent to your doctor who will share the findings with you. It is a good idea to take a loved one with you for support just in case. It may be useful to take along a take a note pad or record the appointment to ensure you have a way to remember important information.
Did you know you can keep track of important information from appointments using features in the OWise diary? Take notes, record audio, and store photos that you can refer back to at any time.
If it is found that you do not have breast cancer your doctor may decide that short-term monitoring is needed. This can be done through physical examination or imaging tests.
If your results confirm that you have breast cancer further tests are needed to determine more information about the cancer, such where it is and how big it is, to enable your care team to develop an appropriate treatment plan.
“Everything is temporary. No good or bad feeling lasts forever. I know that you feel like a rabbit in headlights right now but slowly you will start sleeping a bit better again, you will have your treatment plan which will focus you, and one day at a time you will get through. – Carly Moosah, Breast Cancer Survivor
If you have just been diagnosed with breast cancer, have a read of our blog written by Carly Moosah that lists the 15 things she wish she knew when she was first diagnosed with breast cancer.
Further testing after a breast cancer diagnosis
There are a range of tests available that can be done after you receive a cancer diagnosis to obtain more information about the cancer. Common tests include:
Checking the lymph nodes
The lymph nodes surrounding the breast are common sites for cancer spread. Evaluating these nodes help to determine the extent of disease and informs treatment decisions. Ways to check the lymph nodes include:
- Sentinel lymph node biopsy (SLNB) – removal of a few lymph nodes that cancer is most likely to spread to
- Axillary lymph node biopsy (ALNB) – removal of more lymph nodes from the armpit
Blood tests
Blood tests are useful to check your general health and organ function. Additionally, tumour marker tests can be done to detect cancer biomarkers, such as circulating tumour cells or proteins. These tests can provide information that can help in treatment planning.
CT scan
Computerised tomography (CT) scan is a type of X-ray that produces a 3D image of the inside of the body. CT scans can help to determine where the cancer is, how big it is and how close it is to organs.
MRI scan
An MRI scan can produce clear images throughout the whole body and can be used to locate a tumour, determine its size and check whether it has spread.
PET scan
Positron emission tomography (PET) scans highlight areas of the body where cells are using more energy through injection with a slightly radioactive material. This can often indicate the presence of cancer cells. It can be used to see if the cancer has spread to the lymph nodes or other parts of the body.
PET-CT scan
This combines CT and PET scans to give more detailed information about the cancer.
Bone scan
Bone scans are a technique used to create images of the bones. This can be done when you are initially diagnosed to ensure your bones are healthy. Additionally, bone scans may be recommended during or after treatment to determine whether the cancer has spread to the bones.
What happens after the tests?
The information gathered from the various tests and scans is used by a multidisciplinary team (MDT) to produce a treatment plan tailored to you. A multidisciplinary team can include a surgeon, clinical oncologist (cancer doctor), radiologist (scan specialist), pathologist (lab specialist), plastic surgeon, breast cancer nurse and other healthcare professionals.
Early breast cancer detection and diagnosis is key
Getting an early diagnosis is one of the most influential aspects of a reducing breast cancer related deaths15. We hope that this blog was useful and made you more aware of checking your breasts, what to look our for and how breast cancer is diagnosed.
Keep an eye out for the later blogs in the series that will cover understanding your diagnosis, managing life with breast cancer and the treatment planning process.
We hope that you now better understand how to be breast aware, the signs of breast cancer and the process of how breast cancer is diagnosed. At OWise, we want to make sure you are kept informed so make sure to follow our Instagram and Twitter for any updates. Any questions? Get in touch!
References
- Arnold M, Morgan E, Rumgay H, Mafra A, Singh D, Laversanne M, Vignat J, Gralow JR, Cardoso F, Siesling S, et al. Current and future burden of breast cancer: Global statistics for 2020 and 2040. The Breast. 2022;66(66). doi:https://doi.org/10.1016/j.breast.2022.08.010
- American Cancer Society. Survival Rates for Breast Cancer. www.cancer.org. 2023. https://www.cancer.org/cancer/types/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html
- NHS. How should I check my breasts? NHS. 2018 Jun 27 [accessed 2021]. https://www.nhs.uk/common-health-questions/lifestyle/how-should-i-check-my-breasts/
- Mayo Clinic. Breast self-exam for breast awareness . www.mayoclinic.org. 2022. https://www.mayoclinic.org/tests-procedures/breast-exam/about/pac-20393237#:~:text=Sit%20or%20stand%20shirtless%20and
- National Breast Cancer Foundation. Breast Self-Exam. National Breast Cancer Foundation. 2023. https://www.nationalbreastcancer.org/breast-self-exam/
- World Health Organization. Breast cancer. www.who.int. 2021 Mar 26. https://www.who.int/news-room/fact-sheets/detail/breast-cancer
- CoppaFeel. How To Check Your Breasts, Pecs or Chest. CoppaFeel. https://coppafeel.org/breast-cancer-info-and-advice/how-do-i-check/
- Mayo Clinic. Breast lump: Early evaluation is essential. Mayo Clinic. 2022. https://www.mayoclinic.org/healthy-lifestyle/womens-health/in-depth/breast-lump/art-20044839
- NHS Digital. NHS Breast Screening Programme, England 2021-22. NHS Digital. 2023. https://digital.nhs.uk/data-and-information/publications/statistical/breast-screening-programme/england—2021-22#
- Department of Health and Social Care, NHS England, Whately MP H. New breast cancer screening units to speed up diagnosis. GOV.UK. 2023. https://www.gov.uk/government/news/new-breast-cancer-screening-units-to-speed-up-diagnosis#:~:text=Continued%20investment%20in%20mobile%20breast
- Duffy S, Vulkan D, Cuckle H, Parmar D, Sheikh S, Smith R, Evans A, Blyuss O, Johns L, Ellis I, et al. Annual mammographic screening to reduce breast cancer mortality in women from age 40 years: long-term follow-up of the UK Age RCT. Health Technology Assessment. 2020;24(55):1–24. doi:https://doi.org/10.3310/hta24550
- NHS Choices. Diagnosis – Breast cancer in women. NHS. 2019. https://www.nhs.uk/conditions/breast-cancer/diagnosis/
- American Cancer Society. Mammogram Results | Understanding Your Mammogram Report. www.cancer.org. 2022. https://www.cancer.org/cancer/types/breast-cancer/screening-tests-and-early-detection/mammograms/understanding-your-mammogram-report.html
- Mayo Clinic. Breast biopsy – Mayo Clinic. www.mayoclinic.org. 2021. https://www.mayoclinic.org/tests-procedures/breast-biopsy/about/pac-20384812
- Wang L. Early Diagnosis of Breast Cancer. Sensors. 2017;17(7):1572. doi:https://doi.org/10.3390/s17071572
